Why would toenail fungus linger or recur after treatment?
The condition of onychomycosis (better known as nail fungus) can present itself in several different ways. Where there is toenail fungus, there is also a constant portal of infection to the skin. Overproduction of the sweat glands (hyperhidrosis) provides a breeding ground for fungal infection as fungi multiply in moist, wet, and dark conditions.
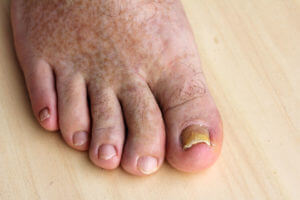
Older individuals are generally more prone to contracting nail fungus. However, at any age, a lowered immune system, chemotherapy, diabetes, and even wearing boots to work every day can heighten your susceptibility. Therefore, it is highly recommended to have a physician assess your condition.
Portions of your toenail will often turn white, yellow, black, brown, or any combination of these. The nail can become fragile and crack, or thicken and form crumbly-like debris underneath the nail plate. Eventually, your nail may detach from its nail bed and fall off.
However, there are other severe conditions that may cause the toenail to discolor and/or thicken; such as melanoma and nail root damage. Having 1 or 2 fungal toenails that have been present over a year without spreading to the other toenails is indicative of nail root damage. Another red flag for damage to your nail root would be if a previously prescribed treatment helped the condition, only to have it return shortly thereafter.
The nail root is located under the proximal nail fold, and it can be damaged from:
- an object falling on the toe
- a toe fracture
- stubbing your toe
- wearing shoes that are too short or narrow
- hiking downhill with poor fitting boots
- events such as running a marathon
- a discolored toenail which bled under the nail and fell off
In these instances, a nail avulsion followed by twice-daily applications of an athlete’s foot cream until the nail has grown in is the standard treatment. If the nail grows back in thick and/or discolored then the root is permanently damaged. Options at this point are to do nothing, have a permanent nail removal, or, if you like to polish your nails, you may trim the nail very short and have an acrylic nail applied.
OTC treatments will rarely eradicate the infection but may help with symptoms by thinning out a toenail that has thickened due to a fungal infection. There are several antibacterial prescription medications; such as topical Penlac and oral Lamisil. Medications all have potential side effects so making an appointment with a podiatrist to find out the best treatment for you is highly recommended.
In-office procedures are available at Salt Lake City Podiatry as well, such as nail removal and laser treatments. A nail avulsion would be a definitive treatment if there are only 1 or 2 toenails affected. Note that laser treatments are not covered by health insurance companies.
Why does my ‘athlete’s foot’ keep coming back?
When it comes to identifying and effectively treating a case of athlete’s foot (tinea pedis), it is important to distinguish which form it has taken. A proper medical diagnosis is highly recommended because athlete’s foot symptoms, treatments, and outcomes are multi-faceted.
- Acute athlete’s foot may present with itching, burning pain, and peeling skin between the toes; tiny blisters called pustules that crust over when popped; and a red rash-like distribution surrounding the perimeter of the foot. Many OTC treatments work for these skin fungal infections, but only if they are used correctly, twice daily for 6 weeks. If you merely stop treating acute athlete’s foot because your symptoms have disappeared, the infection will recur!
- Chronic athlete’s foot infections present in 2 different forms. Most common is the interdigital type which occurs between the toes; manifesting as scales, fissures (small tears), and skin maceration (prolonged saturation). Alternatively, the ‘moccasin variety’ of chronic athlete’s foot is caused by a parasitic fungus that colonizes in layers of dead skin. It presents as dry, silvery, calloused scales on the soles of the feet that may extend up the sides as well.
Athlete’s foot is not only prevalent amongst sports enthusiasts, it is a highly contagious fungal infection commonly seen across the general population. To avoid contracting or transmitting an athlete’s foot, Dr. Elizabeth Auger recommends that you wear footwear at all times during your activities with friends, family, or at the gym.
Chronic skin fungal infections may persist for years, and consequently should be diagnosed by a podiatrist who will prescribe the proper medications and treatment.
What is causing my feet to smell?
The density of sweat glands in our feet (125,000 each) is greater than all other areas of the body, armpit included. Fungus thrives in dark, moist environments and is apt to infect the skin when allowed to linger in damp socks and overworn shoes.
Foot odor is commonly associated with athlete’s foot or abnormally excessive sweating (hyperhidrosis). Both conditions may occur simultaneously, and emit a foul-smelling stench as the bacteria from your sweat breaks down.
Dr. Elizabeth Auger shares her recommendations for getting rid of the malodor:
- Wear synthetic socks that will wick moisture away from your skin. Cotton socks tend to hold onto moisture and prevent the skin from drying.
- Antiperspirant is a treatment for hyperhidrosis. You can try an over-the-counter product and, if the sweat persists, a prescription is available through a physician.
- Alternating your shoes daily will allow them to dry out completely before wearing them again.
- Remove inserts for faster drying; if possible place footbeds in the sunlight.
- Lightly spritz your shoes with white vinegar, or sprinkle baking soda inside them to eliminate the odor.
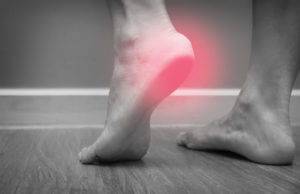
What is making my heel hurt?
Heel pain is one of the most common complaints given for initiating a visit to your local podiatrist. While there are many causes for the pain in your heel, the following conditions are most frequently to blame:
- Plantar fasciitis is inflammation of the plantar fascial band, a large ligament that runs from the heel to the toes and establishes itself as the ‘plantar plate.’ When the arch of the foot lowers (known as overpronation) this band becomes overstretched and inflamed. If the condition becomes ‘chronic’ it can cause the ligament to thicken. Your symptoms along with a physical exam will determine this diagnosis.
Tight calf muscles can be the culprit as they will get cold, stiff, and shorten as you sleep or sit for prolonged periods of time. Long hours spent wearing high heels may also set this disorder in motion. Also, with normal aging, our soft tissue loses its flexibility. The stabbing pain of plantar fasciitis usually starts when you rise and put weight on your feet (as the arch lowers to compensate for that tightness). Once the calf muscles have had a chance to warm up and become more flexible they will offset the pressure on your foot. Stretching these muscles is the best method of eradicating plantar fasciitis, and preventing its recurrence. Foam rolling beforehand gives you added mobility.
- Plantar heel spurs are bone abnormalities that occur when the heel bone (calcaneus) is constantly stressed, causing calcium deposits to build up underneath. These spurs can irritate and compress the inferior calcaneal nerve of the heel, a condition known as Baxter’s nerve, radiating pain to the outside of the foot. Diagnosis can be made with an x-ray.
- A stress fracture of the calcaneus is not associated with direct trauma; such as landing on the heel after a fall. The pain may be aching and dull but can worsen when you’re on your feet a lot. Calcaneus stress fractures are commonly seen in new recruits during boot camp, and when athletes are training for a running event. These activities can put much more stress on the bone than it can handle, so it is best not to increase mileage by more than 10% per week. An MRI is preferred for an accurate diagnosis.
- Plantar fat pad stress syndrome happens in response to prolonged excessive pressure that has been placed on the feet and the pads become irritated. You can feel a lump just under the skin when this occurs. The cushioning these pads are meant to provide can degenerate with age, causing fat pad atrophy. Custom orthotics can help support your feet and heel cups may reduce the impact as you walk.
- Tarsal tunnel syndrome is an entrapment of the posterior tibial nerve as it enters the foot. Sensations such as shooting pain up and down the leg and numbness are common which can be diagnosed with a nerve conduction velocity test. You may reduce the inflammation by resting, elevating your feet, compression, and icing of the areas.