Morton’s Neuroma is one of the most common yet frequently misunderstood causes of foot pain. This condition can transform simple activities like walking or standing into uncomfortable ordeals, yet many people delay seeking help because they’re unsure what’s causing their discomfort.
Morton’s Neuroma is one of the most common yet frequently misunderstood causes of foot pain. This condition can transform simple activities like walking or standing into uncomfortable ordeals, yet many people delay seeking help because they’re unsure what’s causing their discomfort.
Recognizing the signs early and seeking proper treatment can make a significant difference in outcomes and quality of life. Dr. Elizabeth Auger, a trusted foot health expert, emphasizes that understanding this condition is the first step toward finding relief.
With the right approach, most patients can return to their daily activities without persistent pain.
What Is Morton’s Neuroma?
Morton’s Neuroma is a painful condition affecting the ball of the foot, most commonly occurring in the space between the third and fourth toes. Despite its name suggesting a tumor, Morton’s Neuroma isn’t actually a growth, it’s a thickening of the tissue surrounding one of the nerves leading to your toes.
This nerve thickening develops when the tissue around a digital nerve becomes irritated and inflamed, often due to compression or repeated trauma. Over time, the body responds to this irritation by building up fibrous tissue around the nerve, which creates a benign but painful enlargement.
The result is a condition that can cause significant foot nerve pain and interfere with mobility.
The precise mechanism involves the interdigital nerves that run between the metatarsal bones. When these nerves are repeatedly squeezed or irritated, they become swollen and eventually develop the characteristic thickening that defines Morton’s Neuroma.
Who Is at Risk of Morton’s Neuroma?
While anyone can develop Morton’s Neuroma, certain factors significantly increase the likelihood of experiencing this condition.
- Sex: Women are far more likely to develop Morton’s Neuroma than men, with some studies suggesting they’re affected up to five times more frequently.
- Age: The condition typically appears in adults between the ages of 30 and 60.
- Footwear: High-heeled shoes represent one of the most significant risk factors. Similarly, shoes with narrow or pointed toe boxes force the toes into unnatural positions and increase pressure on the interdigital nerves.
- Physical Activity: Athletes and active individuals face elevated risk as well, particularly those engaged in activities involving repetitive stress to the forefoot.
- Runners, for example, repeatedly push off with their toes, while court sport athletes make frequent lateral movements that stress the front of the foot.
- Ballet dancers and those who spend long periods on their feet professionally also experience higher rates of the condition.
- Foot Structure: Congenital problems and foot injuries can both contribute to Morton’s neuroma.
Signs and Symptoms of Morton’s Neuroma
Morton’s Neuroma doesn’t always announce itself dramatically. Symptoms often begin subtly and progress over time, which is why many people initially dismiss their discomfort as general foot fatigue.
- Tingling and Numbness: Tingling or numbness in the toes is frequently among the earliest symptoms. Many patients describe a sensation similar to having their foot “fall asleep,” except it occurs without any obvious cause, like sitting in an awkward position.
- Pain: Burning, sharp, or shooting pain in the ball of the foot is another hallmark symptom. This pain may come and go initially, but often becomes more persistent as the condition progresses.
- Unusual Pressure: One of the most distinctive symptoms is the sensation of standing on a pebble or having a stone in your shoe. This phantom sensation results from the enlarged nerve creating abnormal signals.
Symptoms typically worsen with certain activities or conditions. Walking, especially for extended periods, often intensifies the pain. Wearing tight, narrow, or high-heeled shoes almost invariably aggravates symptoms.
Many patients find temporary relief by removing their shoes, massaging the affected area, or avoiding activities that stress the forefoot.
When to See a Podiatrist for Your Symptoms
Knowing when to seek professional evaluation can prevent a minor issue from becoming a chronic problem.
If you’ve experienced foot pain, numbness, or unusual sensations for more than a few days, it’s worth scheduling an appointment with a podiatrist. This is particularly true if your symptoms interfere with normal activities, don’t improve with rest, or keep recurring even after you’ve modified your footwear.
When caught early, the condition often responds well to conservative treatments. However, if left untreated, the nerve damage can progress, potentially leading to permanent nerve changes that are more difficult to address.
Morton’s Neuroma Treatment Options
The good news about Morton’s Neuroma is that multiple effective treatment options exist, ranging from simple lifestyle modifications to surgical intervention when necessary.
Non-Surgical Treatments
Non-surgical treatments form the foundation of Morton’s Neuroma management and prove successful for many patients. For mild cases, custom orthotic devices can redistribute pressure away from the affected nerve, providing relief while you walk.
Footwear modifications, switching to shoes with wider toe boxes, lower heels, and adequate cushioning, can dramatically reduce symptoms. Physical therapy exercises designed to stretch and strengthen the foot may also help alleviate pressure on the nerve.
Surgical Treatments
When conservative measures provide insufficient relief, minimally invasive options offer the next level of treatment. Corticosteroid injections can reduce inflammation around the nerve, often providing weeks or months of relief.
Some patients benefit from a series of injections over time. Nerve blocks using local anesthetics can also help manage pain, and some practitioners use alcohol sclerosing injections to gradually deaden the affected nerve.
Surgical intervention becomes an option when other treatments fail to provide adequate relief. The most common procedure involves removing the affected portion of the nerve (neurectomy), though some surgeons prefer techniques that release the ligament pressing on the nerve without removing nerve tissue.
Surgery is typically performed on an outpatient basis, and most patients can return to normal footwear within several weeks.
Preventing Morton’s Neuroma
While not all cases of Morton’s Neuroma can be prevented, several strategies can significantly reduce your risk and help maintain long-term foot health.
Choosing Correct Footwear
The shoes you wear play a pivotal role in determining your risk for Morton’s Neuroma. Thoughtful footwear selection is one of the most effective preventive measures available.
Prioritize shoes with a wide toe box that allows your toes to spread naturally without being squeezed together. When trying on shoes, ensure there’s adequate space (roughly a thumb’s width) between your longest toe and the end of the shoe.
Your toes should be able to wiggle freely without pressing against the sides or top of the shoe.
Avoid high heels whenever possible. Heels exceeding two inches shift your body weight forward onto the ball of the foot, dramatically increasing pressure on the interdigital nerves.
If heels are necessary for work or special occasions, limit the duration you wear them and consider bringing comfortable flats to change into.
Exercise and Lifestyle
Regular physical activity promotes overall foot health, but the type and intensity of your activities matter when it comes to preventing Morton’s Neuroma.
Incorporate stretching into your daily routine. Calf stretches help maintain flexibility in the Achilles tendon and reduce strain that can transfer to the forefoot.
Toe stretches, gently pulling the toes apart and holding for several seconds, can help counteract the compressive effects of wearing shoes all day. Stretching the plantar fascia by rolling your foot over a tennis ball or frozen water bottle keeps the tissues supple and promotes healthy circulation.
Strengthening exercises for the intrinsic foot muscles improve stability and biomechanics. Simple exercises like picking up marbles with your toes, scrunching a towel under your foot, or spreading your toes as wide as possible help build the small muscles that support proper foot function.
Stronger feet are more resilient to the stresses that contribute to nerve irritation.
Be mindful of repetitive stress from high-impact activities. If you run, play tennis, or engage in other sports that stress the forefoot, ensure you’re wearing appropriate sport-specific footwear with adequate cushioning.
Increase training intensity gradually rather than making sudden changes that shock your feet. Cross-training with lower-impact activities like swimming or cycling gives your feet periodic rest while maintaining cardiovascular fitness.
Paying Attention to Warning Signs
Perhaps the most important preventive measure is developing awareness of your body’s signals and responding promptly when something feels wrong. While symptoms might resolve on their own, their presence indicates that something is irritating the nerve, and that irritation can progress if the underlying cause isn’t addressed.
When you notice early symptoms, take immediate action. Remove constrictive footwear and switch to more accommodating shoes. If symptoms persist for more than a few days despite self-care measures, or if they recur repeatedly even after you’ve modified your footwear and activities, schedule a professional evaluation.
Take the First Step to Treat Morton’s Neuroma With Dr. Elizabeth Auger, DPM
Morton’s Neuroma is a treatable condition, but outcomes improve significantly when the condition is recognized and addressed early. The distinctive symptoms, tingling and numbness in the toes, sharp pain in the ball of the foot, and the sensation of standing on a stone, should prompt evaluation rather than be dismissed as ordinary foot fatigue.
If you’re experiencing these symptoms, consulting with a qualified podiatrist can provide answers and relief. Dr. Elizabeth Auger brings expertise and a patient-centered approach to diagnosing and treating Morton’s Neuroma, helping patients find the treatment path that best fits their needs and goals.
Don’t let foot pain limit your activities or diminish your quality of life. Call (801) 396-9743 to schedule an appointment or consultation to discuss your symptoms and explore your options for returning to comfortable, pain-free movement.

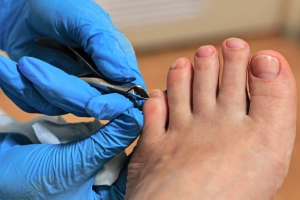 Ingrown toenails rank among the most common, and preventable, foot complaints in podiatric practice. This painful condition occurs when the nail plate grows into the surrounding skin, triggering inflammation and often infection.
Ingrown toenails rank among the most common, and preventable, foot complaints in podiatric practice. This painful condition occurs when the nail plate grows into the surrounding skin, triggering inflammation and often infection. Sesamoiditis is an inflammatory condition affecting the sesamoid bones and surrounding tendons beneath the big toe joint. These tiny bones, embedded within the tendons under the ball of the foot, play a crucial role in normal foot mechanics and weight-bearing activities.
Sesamoiditis is an inflammatory condition affecting the sesamoid bones and surrounding tendons beneath the big toe joint. These tiny bones, embedded within the tendons under the ball of the foot, play a crucial role in normal foot mechanics and weight-bearing activities.