![]()
Same Day Appointments Available!
Call Us 24/7 (801) 619-2170
Salt Lake City * Sandy * West Jordan

Understanding the Different Types of Ingrown Toenails and Their Treatments
Home » Blog » Understanding the Different Types of Ingrown Toenails and Their Treatments
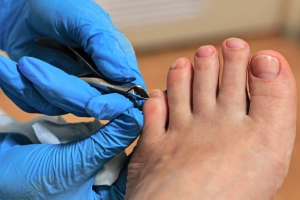 Ingrown toenails rank among the most common—and preventable—foot complaints in podiatric practice. This painful condition occurs when the nail plate grows into the surrounding skin, triggering inflammation and often infection.
Ingrown toenails rank among the most common—and preventable—foot complaints in podiatric practice. This painful condition occurs when the nail plate grows into the surrounding skin, triggering inflammation and often infection.
While teenagers and young adults are particularly susceptible due to hormonal changes that increase sweating and active lifestyles that raise trauma risk, ingrown toenails affect patients across all age groups—including older adults who may face challenges with nail care due to reduced flexibility or underlying health conditions.
Dr. Elizabeth Auger, DPM, brings extensive clinical experience treating ingrown toenails at every stage—from mild cases that respond to conservative care to advanced presentations requiring surgical intervention. Her patient-centered approach emphasizes that accurate identification of type and severity is essential for determining appropriate treatment.
How an Ingrown Toenail Develops
The toenail consists of the nail plate—the visible hard portion—which grows from the matrix beneath the proximal nail fold. The plate sits on the nail bed, bordered on each side by lateral nail folds.
In healthy nail growth, the plate glides forward smoothly without impinging on surrounding tissue.
An ingrown toenail develops when the lateral edge of the nail plate penetrates the adjacent fold. This triggers the body’s inflammatory response, as the embedded nail acts essentially as a foreign body within the tissue.
The area becomes red, swollen, and tender. Left unchecked, this cascade can progress from simple inflammation to bacterial infection, granulation tissue formation, and chronic wound complications.
Distinguishing true ingrown nails from conditions like paronychia, fungal nail dystrophy, or subungual exostosis ensures accurate diagnosis and appropriate treatment.
Types of Ingrown Toenails
Stage 1: Mild Ingrown Toenail
Stage 1 represents the earliest phase of an ingrown toenail and offers the best opportunity for conservative management. The nail edge presses into the lateral fold, producing tenderness, mild redness, and slight swelling—particularly when wearing shoes or applying direct pressure.
Stage 1 nails have not yet progressed to infection; no drainage, pus, or discharge is present. Common triggers for mild ingrown toenails include improper trimming, tight shoes, and minor trauma from athletic activity.
When addressed promptly, Stage 1 nails typically resolve within two to twelve weeks.
Stage 2: Moderate Ingrown Toenail
Stage 2 signals significant escalation and indicates that conservative home care alone may no longer be sufficient. The inflammatory process has intensified, and bacterial infection has typically begun.
Patients experience increased pain that may interfere with walking, marked redness, and substantial swelling. The hallmark of Stage 2 is seropurulent drainage—a mixture of fluid and pus seeping from where the nail penetrates the skin.
Medical evaluation becomes particularly important because infection can spread without appropriate intervention. Patients with diabetes or compromised circulation face elevated complication risks and should seek prompt care.
Stage 3: Severe Ingrown Toenail
Stage 3 represents chronic, advanced ingrown toenail disease requiring definitive intervention. Patients at this stage have typically experienced symptoms for months during which infection has become established.
The inflammatory response has produced hypertrophic granulation tissue—sometimes called “proud flesh”—which grows over the nail edge, bleeds easily, and prevents the nail from correcting its growth pattern. There is significant swelling, chronic purulent discharge, and marked lateral wall hypertrophy.
Surgical intervention is generally most effective for Stage 3 disease, as these anatomical changes cannot resolve with conservative measures alone.
Nail Shape–Related Ingrown Toenails
Some patients develop ingrown toenails due to inherent nail shape rather than external factors. Pincer nails—also called trumpet nails—are characterized by excessive transverse curvature that causes the lateral edges to curve downward and inward, sometimes until they nearly meet beneath the nail.
This creates a pinching effect causing pain even without true nail penetration.
Causes include hereditary factors, tight footwear, fungal infections, and arthritic bone changes affecting the toe. Managing shape-related ingrown nails requires addressing the underlying deformity through specialized bracing, partial nail avulsion with matrixectomy, or correction of bone abnormalities.
Underlying Causes and Risk Factors
Understanding the factors that contribute to ingrown toenails helps patients take preventive action.
- Improper trimming habits—cutting nails too short, rounding the corners, or tearing nails—represent the most modifiable risk factor.
- Tight shoes, pointed toe boxes, and high heels compress the toes and force the nail against the lateral folds.
- Repetitive pressure from athletic activities and work environments requiring safety boots also contribute.
- Direct trauma to the toe can damage the nail bed and alter growth patterns.
- Hyperhidrosis, or excessive sweating, softens periungual skin and creates an environment favorable to bacterial growth.
- Fungal nail infections change nail texture and shape in ways that predispose to ingrowth.
- Genetic factors influence nail curvature and thickness.
In addition to these direct causes, certain patient populations face elevated risks:
- Individuals with diabetes may have reduced sensation that delays recognition and impaired healing.
- Those with peripheral vascular disease lack adequate blood flow.
- Immunocompromised patients cannot mount effective responses to infection.
Treatment Options Guided by Severity
Conservative Treatments for Mild Cases
Mild Stage 1 ingrown toenails often respond to conservative home care.
Soak the affected foot in warm, soapy water for ten to twenty minutes, three to four times daily—this softens tissue and reduces inflammation. After soaking, gently elevate the nail edge using cotton or dental floss, replaced daily.
Apply topical antiseptic and allow thorough drying before putting on footwear. Wear open-toed shoes or those with wide toe boxes.
However, conservative treatment is not appropriate for all cases. Patients should not attempt self-treatment if:
- they have diabetes, peripheral vascular disease, or immune compromise
- infection signs are present; if symptoms persist beyond one to two weeks of proper care
- the condition recurs repeatedly.
In-Office Treatments for Moderate Cases
Stage 2 ingrown toenails benefit from professional intervention. With the patient under local anesthesia, doctors can perform nail lifting techniques—carefully separating the ingrown edge and placing material such as cotton or a gutter splint beneath to maintain separation.
Gutter splints provide immediate pain relief by preventing the nail from contacting inflamed tissue. When infection is present, debridement removes infected tissue and drains any abscess.
Importantly, oral antibiotics are generally not necessary for localized infections when the underlying cause is addressed; they’re reserved for spreading cellulitis.
Surgical Solutions for Severe or Recurrent Cases
Stage 3 and recurrent cases require surgical intervention.
Partial nail avulsion removes only the ingrown portion—typically one-sixth of the nail width—while preserving the remainder. This provides immediate relief but carries recurrence risk. For permanent resolution, partial avulsion is combined with matrixectomy—destruction of the lateral nail matrix to prevent regrowth.
Chemical matrixectomy using phenol has been the gold standard for decades, with the chemical applied to destroy nail-producing cells. Sodium hydroxide offers an alternative with potentially faster healing, while trichloroacetic acid has emerged as another effective option.
All three show similar success rates.
Surgical matrixectomy using sharp excision is reserved for cases where chemical methods are contraindicated. Recovery typically involves one to two days of rest, with patients returning to work within days.
Complete healing occurs within two to six weeks, and the resulting nail appears cosmetically normal.
Prevention and Long-Term Foot Health
Here are some common recommendations for maintaining your toes and avoiding ingrown toenails:
- Trim Toenails Properly: Cut toenails straight across—never rounding corners—and leaving them long enough that corners extend past the lateral folds. Trim when softened, using proper toenail clippers.
- Wear Proper Footwear: Choose shoes with adequate toe room, approximately half an inch between the longest toe and shoe tip. Avoid pointed-toe shoes and excessively high heels.
- Practice Foot Hygiene: Keep feet clean and dry, inspect nails regularly, and treat fungal infections promptly. Those with diabetes or circulation problems should inspect feet daily and seek professional evaluation for any nail abnormalities.
When You Should See a Podiatrist
Red flags requiring prompt attention include pus or discharge, red streaks extending toward the foot, fever, significant swelling involving the entire toe, severe pain limiting walking, and skin growing over the nail. Symptoms persisting beyond one to two weeks of proper home care, or worsening despite treatment, warrant evaluation.
Patients with diabetes, peripheral vascular disease, or immune compromise should never attempt self-treatment for ingrown toenails.
Take the First Step Toward Healthy, Pain-Free Feet
Ingrown toenails are highly treatable at every stage—from the earliest discomfort to chronic cases persisting for months. Do not wait until pain interferes with daily activities, infection spreads, or you can no longer wear normal shoes.
Early intervention leads to faster healing, less discomfort during treatment, and better long-term outcomes.
Dr. Elizabeth Auger, DPM, provides expert evaluation and personalized treatment plans for patients experiencing ingrown toenails at any stage. Whether you need guidance on proper nail care, in-office procedures to address an active problem, or surgical treatment for recurrent or severe disease, Dr. Auger combines technical expertise with compassionate care to help you achieve healthy, pain-free feet.
Schedule your appointment today by calling (801) 396-9743 and take the first step toward lasting relief.
Foot and Ankle
Conditions
- Allergic Contact Dermititis
- Achilles Tendonitis
- Athlete’s Foot
- Brachymetatarsia
- Bunions
- Calluses
- Diabetes
- Flatfoot (Fallen Arches)
- Foot Ulcerations (Diabetic Ulcers/Wounds)
- Salt Lake City Fungal Nail
- Ganglions
- Gout
- Haglund’s Deformity
- Hallux Rigidus
- Hammertoes
- Heel Pain (Fasciitis)
- Foot Infections
- Ingrown Toenails
- Injuries
- Metatarsalgia
- Morton’s Neuroma
- Osteoarthritis
- Paronychia
- Plantar Fasciitis
- Plantar Warts
- Posterior Tibial Dysfunction
- Rheumatoid Arthritis
- Running Injuries
- Sesamoiditis
- Skin Conditions
- Sprains & Strains
- Tailor’s Bunion
- Tarsal Tunnel Syndrome
- Tendonitis
- Toe Deformities
- Xerosis
1561 W 7000 S, Suite 200
West Jordan, Utah 84084
(801) 509-9959
3934 S 2300 E,
Salt Lake City, UT 84124
(801) 396-9743
